What is the pancreas?
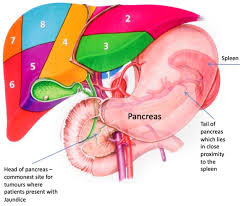
The pancreas is a spongy organ approximately 12-15cm in length and lies behind the stomach (see diagram below). The pancreas consists of a head, neck, body, tail and also a portion below the head called the uncinate process. The main functions of the pancreas are; the production of the hormone insulin, which controls blood sugar levels, and the production of pancreatic juices, which pass through the main pancreas duct into the small intestine to digest food.
What are the common types of pancreas tumours?
Types of pancreas tumours include:
- Adenocarcinoma (commonest)
- Neuroendocrine tumour
- Cystic tumours
- MEN Syndromes
- Insulinomas and Gastrinomas
The large majority of pancreatic tumours are adenocarcinoma, and most are not amenable to surgical treatment. Surgery is offered dependent upon the locality of the tumour and the fitness of the patient to undergo major surgery.
What is pancreas cancer?
Pancreatic cancer is the sixth most common cancer in the U.K. Like any cancer its true cause is unknown, but the risk factors are increasing age, drinking excessive amounts of alcohol over many years and smoking. Pancreas cancer is actually two to three times more common in smokers.
How does Pancreas Cancer present?
Pancreas Cancer presents commonly with symptoms described as:
‘Painless, obstructive jaundice’, ‘weight loss’, ‘poor appetite’
Pancreas cancer has no specific symptoms, presenting with little or no pain in most patients. Some patients describe a feeling of abdominal discomfort, but most patients eventually notice a change in colour of the white of their eyes (sclera) to a yellow tinge – jaundice. Jaundice is associated with very dark urine (tea without milk) and pale stools (yellow/grey or clay coloured, floating foul-smelling stool). Other symptoms are typical of a suspected malignancy, such as weight loss, poor appetite and general deterioration in health. Occasionally patients can also complain of back pain, this can occur with tumours located to the body or tail of the pancreas.
Diagnosis
The diagnosis of pancreatic cancer is made following a careful consultation with your specialist surgeon who will examine you and order certain specialised blood tests. Computed Tomography (CT) scanning forms an important part of diagnosing pancreas cancer by providing detailed pictures/ images. Magnetic Resonance Imaging (MRI) can also be used. You may also need an Endoscopic Ultrasound Scan (EUS) and Endoscopic retrograde cholangiopancreatography ERCP.
ERCP, is a special x-ray of the common bile duct (see diagram). Similar to gastroscopy, a flexible tube (endoscope) is passed down the patient's throat through the stomach and into the duodenum (small intestine). Pictures on x-ray of the common bile duct and pancreas duct can be taken by injecting a dye into the ducts.
EUS is a procedure that allows careful examination of the pancreas and is very accurate at diagnosing pancreatic cancer. As for ERCP an endoscope is passed with EUS having a special adapted ultrasound probe on the end, which scans the pancreas for cancers and is able to take biopsies. This procedure is especially useful for examining smaller cancers that may not be picked up by a CT scan.
Treatment
Pancreas cancer’s treatment depends on factors such on its size, location on the pancreas (head, body, neck, tail) and evidence of any spread of the cancer. Complete removal of the cancer by surgery is the best and recommended treatment, with other possible treatments including chemotherapy and radiotherapy.
What Surgery is involved?
Head of pancreatic tumours are removed by a procedure called a Whipple’s Pancreaticoduodenectomy. This is major surgery, which involves removing the head of the pancreas along with part of the bile duct, stomach and duodenum. The remaining pancreas, bile duct and stomach are reconstructed using the small bowel. Patients are in hospital for 10-12 days, with recovery at home taking a further four to six weeks. Immediately following surgery for the first 24 to 48 hours patients are managed on the high dependency unit with transfer to their private room for the remainder of their stay.
Laparoscopic Pancreatic Surgery
Laparoscopic ‘keyhole’ surgery is offered to patients with a pancreatic tumour or cysts on the tail of the pancreas. This surgery allows for quicker recovery however, it is only possible in selected cases. The surgery involves the use of four or sometime five small 1-2cm incisions as shown below. The tail of the pancreas is removed through the belly button wound using a small bag.
Effects of Laparoscopic Distal Pancreatectomy
All patients are warned that the spleen as it lies in close proximity to the tail of the pancreas in some cases needs to be removed (see diagram below). The cells that control blood sugar levels predominantly lie on the tail of the pancreas. Hence once the tail of the pancreas has been removed some patients can become insulin resistant, or diabetic following surgery. Laparoscopic pancreatic surgery does lead to quicker recovery with most patients being discharged in 5-7 days.
Incisions used for Laparoscopic Distal Pancreatectomy
What are the effects of Open Pancreas Surgery?
Following a Whipple’s, patients do take time to recover, with a return to normal eating taking in some cases at least one to two months. Patients often lose weight and can complain of persistent nausea after surgery. Regaining a good intake of adequate diet and fluids as well as good wound care are the mainstay of follow up care for patients undergoing surgery for pancreas cancer.
Do all patients have Surgery? - Non-Surgical Treatment
Unfortunately, not all patients are able to undergo surgery for pancreas cancer. Therefore, excellent support for patients is required for the relief of Jaundice, pain control, Oncology and Palliative care support. Patients as well as their families have access to all the care this service provides. Chemotherapy forms the mainstay of treatment of patients with pancreas cancer.
For more information on Pancreatic Cancer, the Pancreatic Cancer UK website has excellent information and support for patients and their relatives.
Diagram of Pancreas
